Fears weight loss jabs could spark a new health crisis as NHS prepares mass rollout

GB NEWS
New research has raised questions about the long-term harm weight loss jabs may pose
Don't Miss
Most Read
A new health crisis could be looming from the side effects of weight loss jabs, experts warn, as the NHS prepares to roll them out to more than a million heart patients.
The NHS has cited a key trial which suggests the drugs can reduce the risk of heart attacks and strokes by around 20 per cent.
But a new analysis of the trial warns the real-world benefit is smaller and needs to be weighed carefully against the risks. It shows tens of thousands could suffer side effects and the bill could run into billions of pounds a year, raising concerns about safety and pressure on the NHS.
Separate research has also found up to 40 per cent of weight loss may come from muscle and bone - not fat, adding to fears about frailty and long-term harm.
The weight loss drug expansion, announced today, would see around 1.2 million people in England offered semaglutide, known as Wegovy, to cut their risk of heart attacks and strokes, following draft guidance from the drug regulator, the National Institute for Health and Care Excellence.
But leading experts say the benefits are more modest than headline figures suggest - while the risks and costs could be substantial.
Professor Carl Heneghan, and Dr Tom Jefferson from Oxford University’s Centre for Evidence Based Medicine, who carried out the analysis said the key trial behind the rollout risks giving a misleading picture of the true benefits and risks.
While the trial reported a 20 per cent reduction in major heart problems, they warned this headline figure exaggerates the real-world benefit.
 Weight loss drugs have sparked fierce debates in recent years | GETTY
Weight loss drugs have sparked fierce debates in recent years | GETTYAround 100 patients would need to be treated to prevent a single heart attack, there was no clear reduction in stroke, and deaths fell only slightly, the analysis found.
“These headline figures can be misleading,” Prof Heneghan said. “When you break them down, the absolute benefits are modest.”
They also raised concerns about how the trial was conducted. “These were highly selected patients who were closely monitored and given intensive care - far beyond what we would expect in routine NHS practice,” Prof Heneghan said.
He added: “They had around 17 follow-up visits over just three years, which is simply not how care is delivered in the real world."
LATEST DEVELOPMENTS
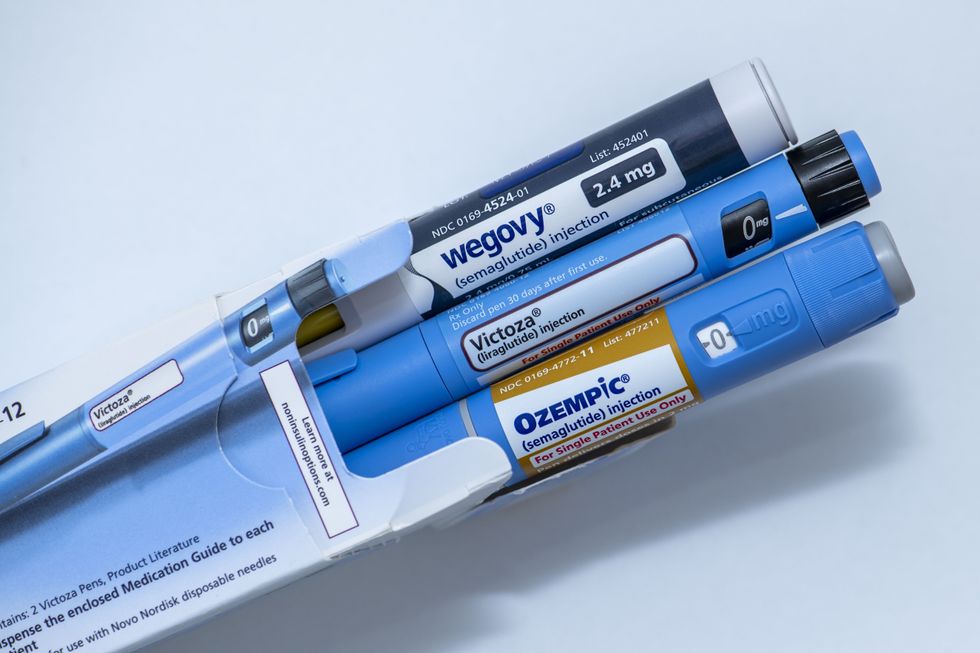 Weight-loss medications such as Ozempic, Wegovy and Mounjaro offer significant health benefits | GETTY
Weight-loss medications such as Ozempic, Wegovy and Mounjaro offer significant health benefits | GETTYHe added: "This is essentially a single industry-funded trial, so we need to be cautious about how widely we apply the findings.”
At the same time, side effects were common. Up to 45 per cent of patients reported gastrointestinal problems such as nausea, vomiting and diarrhoea, while nearly one in five stopped taking the drug due to adverse effects.
“These drugs are not easy to tolerate for a significant proportion of patients,” Prof Heneghan said.
The analysis showed that if 1.2 million people are treated, around 30,000 could stop each year because of side effects, while 60,000 to 80,000 could experience ongoing adverse effects.
The analysis also estimated approximately 1,800 additional cases of gallbladder disease annually.
Separate research shows the drug can also lead to pancreatitis and eye problems.
The researchers also warned of the potential financial burden. NHS drug prices are confidential, but using typical UK pricing as a guide, treatment is estimated at £2,000 to £3,600 per patient a year - meaning a total bill of roughly £2.4billion to £4.3billion annually depending on the price agreed.
This does not include GP visits, monitoring, managing side effects or patients dropping out.
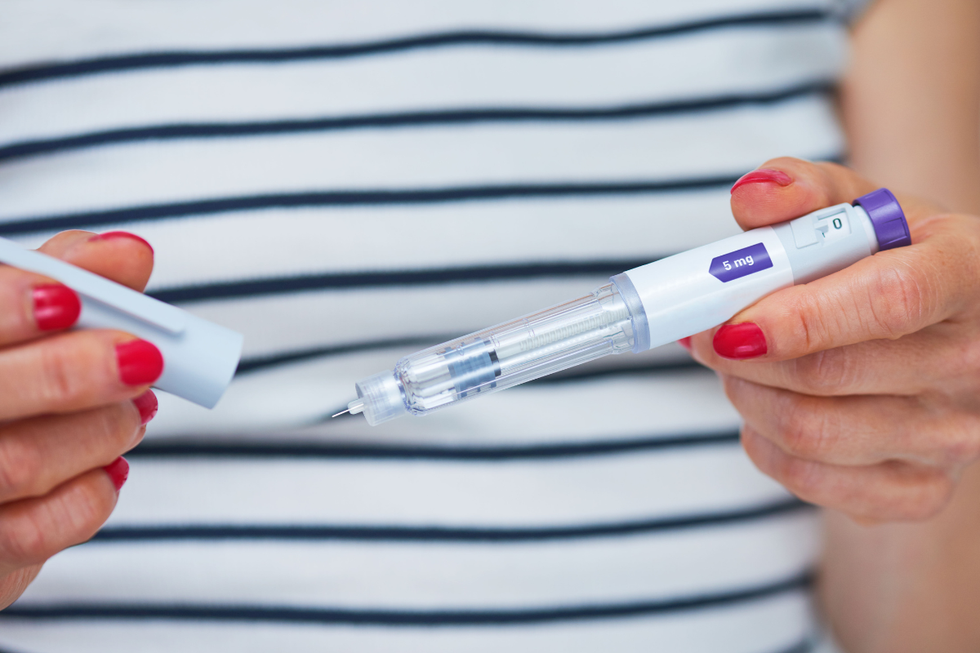
The jab is being rolled out to millions of Britons
| GETTYThe experts say once those are factored in, the true cost could reach £4billion to £5billion a year - similar to major NHS drug budgets, for what they describe as a modest benefit.
Prof Heneghan said: “That is on a scale comparable to major NHS drug programmes, for what is at best a modest absolute benefit.”
Separate scientific research has raised further concerns about loss of muscle and bone mass linked to the drugs.
A review involving researchers at the University of Liverpool found up to 40 per cent of weight lost may come from lean tissue, including muscle and bone.
And a study published in TheLancet found around a quarter to a third of weight loss was linked to loss of muscle and other lean tissue.
Doctors warn this could leave patients weaker, more frail, and more vulnerable to falls and fractures, particularly in later life.
Prof Heneghan said: “Any drug that reduces muscle mass and bone density is a bad idea for people who are vulnerable to frailty, fracture and osteoporosis.”
Physiotherapists say they are already seeing problems emerging in clinics. Hayley Jarvill, a senior physiotherapist specialising in bone health, said patients are reporting joint and tendon issues.
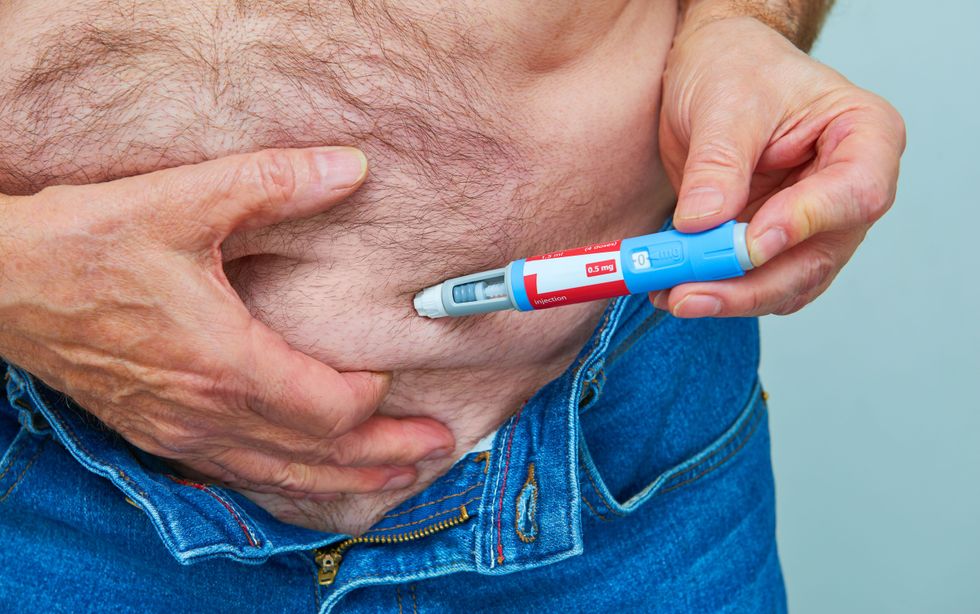 'A reduction in body weight does not automatically mean the person is well-nourished or healthy' | GETTY
'A reduction in body weight does not automatically mean the person is well-nourished or healthy' | GETTY“A lot of people are taking these injections alone and becoming malnourished,” she said. “They are losing muscle mass and then bone mass, and we are seeing reduced strength and stamina.”
Sam Bhide, a spokeswoman from the Chartered Institute of Physiotherapy, warned: “This doesn’t just affect fat - it also affects muscle.
Ms Bhide, clinical director of the physiotherapy group Physiozen added: “If muscles are not strong enough to support the body, we will see new physical problems, particularly affecting the hips, back and spine.”
Currently, the drugs are offered on the NHS mainly to people with obesity through specialist weight management services.
Under the new plans, they would also be given to patients with cardiovascular disease and a BMI over 27, significantly expanding eligibility.
Shirley Hopper, MHRA Deputy Director of Innovative Medicines said: "Our key priority is enabling access to high quality, safe and effective medical products.
"We’re assured that the appropriate regulatory standards of safety, quality and effectiveness for the approval of this medicine have been met. This treatment option that prevents heart disease and strokes is an important step forward in tackling the serious health consequences of obesity.
"As with all medicines, we will keep its safety under close review."
NHS England said the treatment would be prescribed alongside diet and exercise as part of wider care.










