NHS midwives to receive anti-racism training to combat 'national emergency' of maternity deaths

Patrick Christys' head to head on NHS budget soaring but no real change in service |
GB NEWS
All midwifery university courses must update their teaching to include discrimination and racial biases training
Don't Miss
Most Read
Latest
Midwives working in the NHS are to receive anti-racism training to combat the "national emergency" of maternity deaths.
Midwifery university courses are to be overhauled after concerns are growing that discrimination in maternity wards are contributing to higher deaths among Black and Asian mothers.
The Nursing and Midwifery Council (NMC) is planning to integrate anti-racism training during degrees to tackle "systemic" discrimination in maternity.
Reviews into the deaths of mothers and babies, as well as maternity scandals, have pointed to racism being a contributing factor to the avoidable tragedies.
TRENDING
Stories
Videos
Your Say
There has been accounts where Black mothers were denied pain relief by midwives, being called "tough" or "demanding" and told they were better at enduring childbirth.
Maternity deaths, during or after childbirth, have hit their highest levels in 20 years in England, with Black women three times more likely to die than her white counterpart, the Times reports.
Black babies are twice more likely to be stillborn.
The NHS has been notified with 22 safety warnings by official bodies to tackle discrimination in maternity wards over the past 10 years, but the situation is worsening, rather than improving.
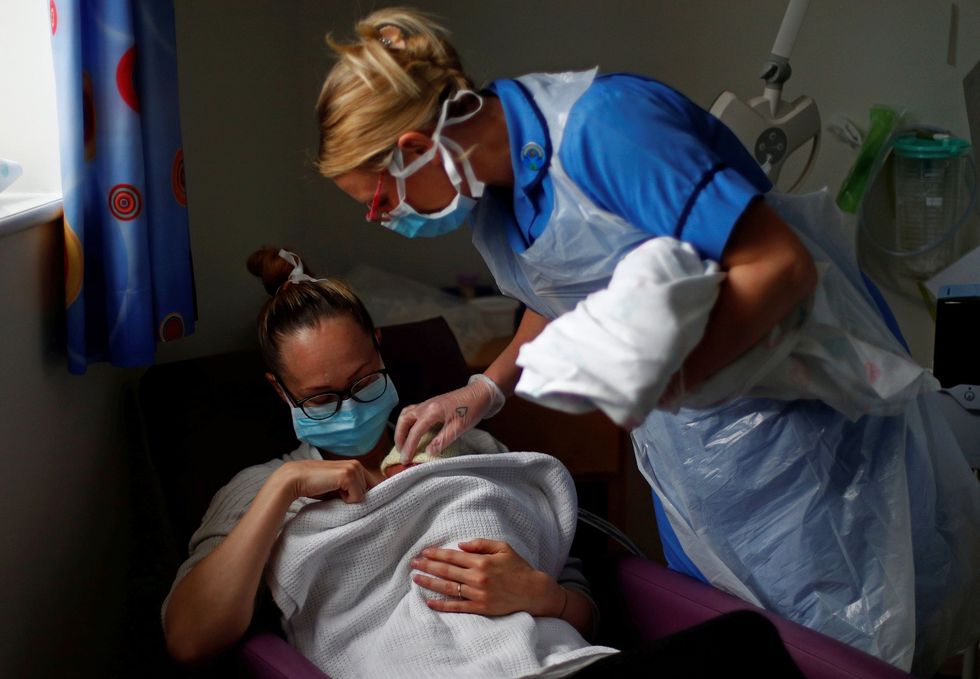
Maternity deaths, during or after childbirth, have hit their highest levels in 20 years in England
|GETTY
All universities teaching midwifery degrees must update their curriculum under the new initiative, ensuring that discrimination and racial biases training is included.
This will come into effect in the next academic year for trainee midwives.
Paul Rees, MBE, Chief Executive and Registrar of the NMC, described the situation as a "national emergency" and racism in maternity wards "compounds the problem".
He said: "Every day, thousands of midwives deliver safe, kind and equitable care that brings joy to women and families across the UK.
LATEST DEVELOPMENTS

Black women three times more likely to die during or after childbirth than their white counterparts
|GETTY
“However, for far too many families, that has not been the case, with absolutely devastating consequences.
“The evidence is clear that racism within maternity services compounds the problem. Black and Asian women are more likely to die during pregnancy or in the immediate postnatal period, and their babies are more likely to be stillborn.
“The situation is totally unacceptable and is a national emergency."
The NMC, who approves and monitors all midwifery programmes throughout the UK, has said it will design a set of principles in the coming weeks, due to be published in late spring.
These anti-racism principles will then be embedded in all university courses by the next academic year.
The NMC will develop such principles with the guidance and advice from Black, Asian and other ethnic minorities who have lived experiences of receiving poor maternity care in the UK.
More broadly, they will also develop a similar set of principles for nursing programmes across the UK.
Sharon Hodgson MP, Public Health Minister, Department for Health and Social Care, welcomes the move from the NMC and said the Government is taking "urgent action" to tackle this issue, including hiring more midwives and establishing a maternity taskforce to deliver "rapid improvements" to the sector.
She said: "The stark disparities in outcomes for Black and Asian mothers and babies are unacceptable, and tackling them is a priority for this government.
"We're taking urgent action to improve maternity services.
"This includes launching an anti-discrimination programme, hiring more midwives, and establishing a new Taskforce - chaired by the Secretary of State - to deliver rapid improvements in maternity and neonatal care, acting on the recommendations from Baroness Amos' independent investigation."
This comes after a report conducted by Baroness Valerie Amos, which found that maternity and neonatal services in England are under severe strain and often failing to provide safe, consistent and compassionate care for families.
Drawing on evidence from thousands of families and staff, the interim report, published in February 2026, highlights widespread issues including staff shortages, capacity pressures, poor leadership, and a fragmented system that leads to unequal care depending on location.
It also identifies serious cultural problems, including a lack of accountability when things go wrong, as well as persistent racism and discrimination that contribute to significantly worse outcomes for Black, Asian, and disadvantaged women.
Families frequently reported not being listened to, experiencing trauma, and facing barriers to transparency after incidents of harm.










