Fresh meningitis outbreak sparks warnings coroners’ reports being ignored

Keeleigh Goodwin speaks to GB News after contracting meningitis on a night out in Kent |
GB NEWS
Vaccination failures have been raised repeatedly in earlier inquests
Don't Miss
Most Read
Vital safety lessons from past meningococcal disease are not being acted on - with researchers saying coroners have raised the same concerns for more than a decade.
Twenty confirmed cases and two deaths linked to meningococcal infection have been reported in Kent this month, in what health officials say is a fast-moving cluster affecting young people.
But analysis by King's College London epidemiologist Dr Georgia Richards, founder of the Preventable Deaths Tracker, suggests the tragedy may not be new - and that repeated failures identified in official death investigations have still not been fixed.
Dr Richards said coroners’ reports show a pattern of missed diagnoses, vaccination gaps and poor communication that has appeared repeatedly in deaths from the disease.
TRENDING
Stories
Videos
Your Say
“These reports are a sobering read,” she said.
“The standout theme across all deaths was the plight of parents who did all they could to raise the alarm about their unwell children. But system failures, human factors, and inadequate public health mechanisms failed the young and vulnerable.”
Her team has launched a live dashboard tracking deaths from meningococcal disease using official coroners’ reports - known as Prevention of Future Deaths (PFD) reports - which are issued when a coroner believes action could stop similar fatalities happening again.
According to the analysis, there were 504 deaths in England and Wales between 2013 and 2024 in which meningococcal infection was recorded as a cause.

Twenty confirmed cases and two deaths linked to meningococcal infection have been reported in Kent this month
|PA
Before the Covid pandemic, there were on average 53 deaths a year, falling to about 26 a year between 2020 and 2024.
However, only a small number of these deaths led to formal warnings from coroners.
Researchers identified 11 deaths investigated in coroner PFD reports since 2013, written by 10 coroners across England and Wales.
Despite representing only a fraction of total deaths, the reports repeatedly highlighted serious failings.
Neglect contributed to five deaths, with one case serious enough to engage Article 2 of the European Convention on Human Rights, because of the number of failures identified.
Missed or delayed diagnosis was one of the most common themes.
In one case, a 21-year-old university student in Kent was seen by both his GP and a hospital but was misdiagnosed with a virus and discharged.
The coroner also found he had not received the MenACWY vaccination, raising concerns about how vaccination programmes were being monitored.
Eight years later, Dr Richards says the same issues appear to remain.
LATEST DEVELOPMENTS:

Dr Richards said the warnings should have been used to prepare for future outbreaks
|PA
“Eight years on, the concerns raised by the coroner in this PFD are starkly relevant for today,” she said.
Vaccination failures were raised repeatedly in earlier inquests.
In 2014, a coroner warned after the death of a five-month-old baby whose third vaccination had been delayed.
In 2017, another report followed the death of a 16-year-old, with the coroner calling for wider vaccination coverage for teenagers at higher risk.
In 2018, just months before the Kent case, a coroner found the system had failed to identify and notify an unvaccinated 18-year-old before she left for university.
Dr Richards said these warnings should have been used to prepare for future outbreaks.
“Using the Preventable Deaths Tracker’s tools, we can rapidly identify similar events where lessons should have been learnt,” she said.“These deaths should have been used by our public health agency to better prepare local communities.”
The data also shows that meningococcal disease overwhelmingly affects the young.
All deaths recorded in coroners’ reports were in people aged between three months and 28 years, with a median age of 15. All had no underlying health problems.
Sepsis was listed as a cause of death in almost every case.
Coroners repeatedly highlighted the same failures across the NHS and emergency services, including poor communication, lack of training, delays in treatment and breakdowns in basic systems.
In one case, a 15-year-old girl was diagnosed with a vomiting bug in A&E and sent home. When her condition worsened, NHS 111 advised an urgent ambulance - but the crew failed to recognise how ill she was and did not take her to hospital. She died days later.
In another, meningococcal septicaemia was missed by ambulance crews and GPs before the death of a six-year-old boy.
No vital signs were recorded, no full examination was carried out, and when his condition worsened, there were no ambulances available, forcing his parents to drive him to hospital themselves.
Dr Richards said such cases show why coroners’ warnings must be taken seriously.
“There were five major concerns raised by coroners in two-thirds of the reports, including poor communication, delays, gaps in training, lapses in the provision of care, and failures in systems and processes,” she said.
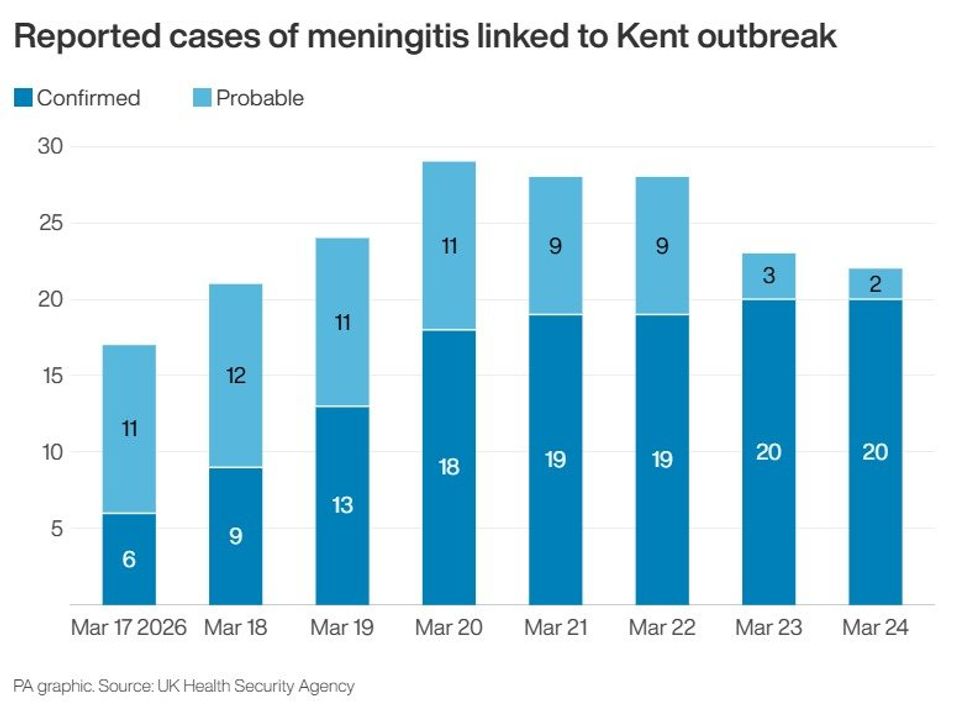
Chart shows reported cases of meningitis linked to Kent outbreak
|PA
Under the law, organisations receiving a coroner’s PFD report must respond within 56 days explaining what action they will take.
But the tracker found responses were often missing or late.
Just four reports had all the required replies, while two-thirds of organisations had overdue responses.
In more than half of cases, coroners sent warnings only to local bodies, even when they believed the problem was national.
After the death of a two-year-old in 2017, one coroner warned: “I am concerned that this is a nationwide issue which warrants consideration by NHS England as the commissioner of primary care services.”
In another case, after the death of a healthy 22-year-old, the coroner said there would be “great merit in sharing the learning nationally” - but no system exists to ensure that happens.
Dr Richards said the latest outbreak should be a wake-up call. “All of these deaths were preventable,” she said.
“So let’s not wait for another outbreak before taking action to prevent future deaths. Time is of the essence.”
An NHS spokesman said: “When you need urgent medical help, NHS 111 call handlers are trained to recognise priority symptoms and respond quickly. Calls can be escalated at any time if new information or concerns arise. NHS 111 is always available for speedy health advice - but if you think you or someone you care for may have symptoms of meningitis, such as a high fever, headache or rash, call 999 or go to your nearest A&E immediately.”
“Free vaccines to protect against meningitis are available through the NHS routine immunisation programme. If your child has not yet been vaccinated, please contact your GP practice to arrange an appointment.”