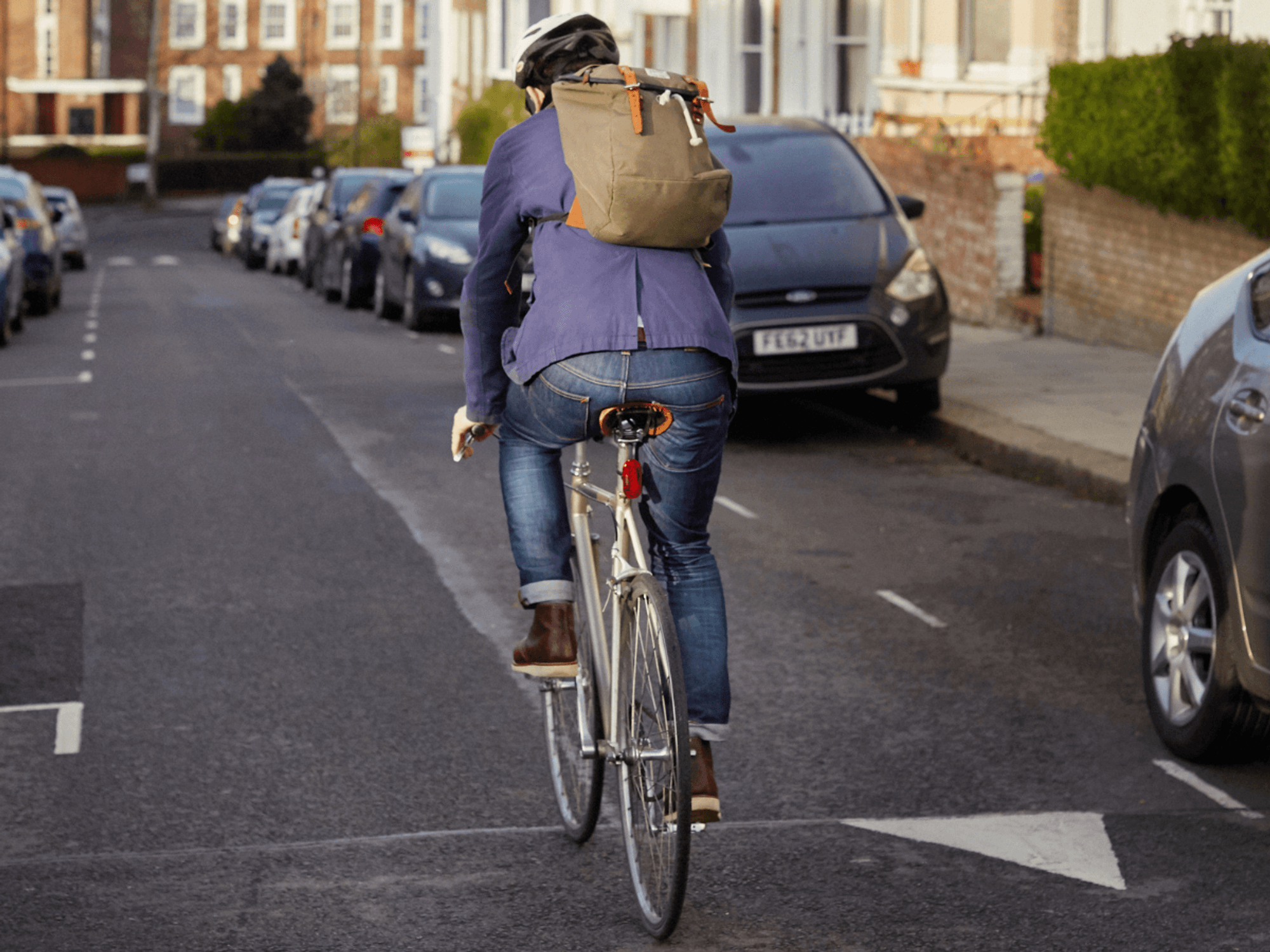Corridor care now routine across NHS, safety watchdog warns

GB News
The investigation found stark differences in how hospitals are responding
Don't Miss
Most Read
Trending on GB News
Unsafe “corridor care” - once seen as a last resort during winter NHS crises - is now routinely used throughout the year, a major safety investigation has warned.
In the first major report of its kind, the Health Services Safety Investigations Body (HSSIB) has found patients across England are regularly being treated in corridors, waiting rooms and other makeshift spaces because hospitals no longer have the capacity to cope with demand.
The watchdog warns this normalisation of corridor care carries serious patient safety risks - including missed deterioration, delayed emergency responses, infection risk, and lack of access to basic equipment such as piped oxygen.
In some cases, there are no emergency call bells at all.
The investigation concludes that what was once considered unacceptable is now embedded in everyday NHS practice.
Unlike previous reports, the HSSIB investigation found corridor care is no longer confined to winter pressures.
Investigators visited hospitals between August and December 2025 and found all were already relying on temporary care environments because of persistent pressure on beds, staff, and patient flow.
The report states there is now “no longer significant seasonal variation” in corridor care use.
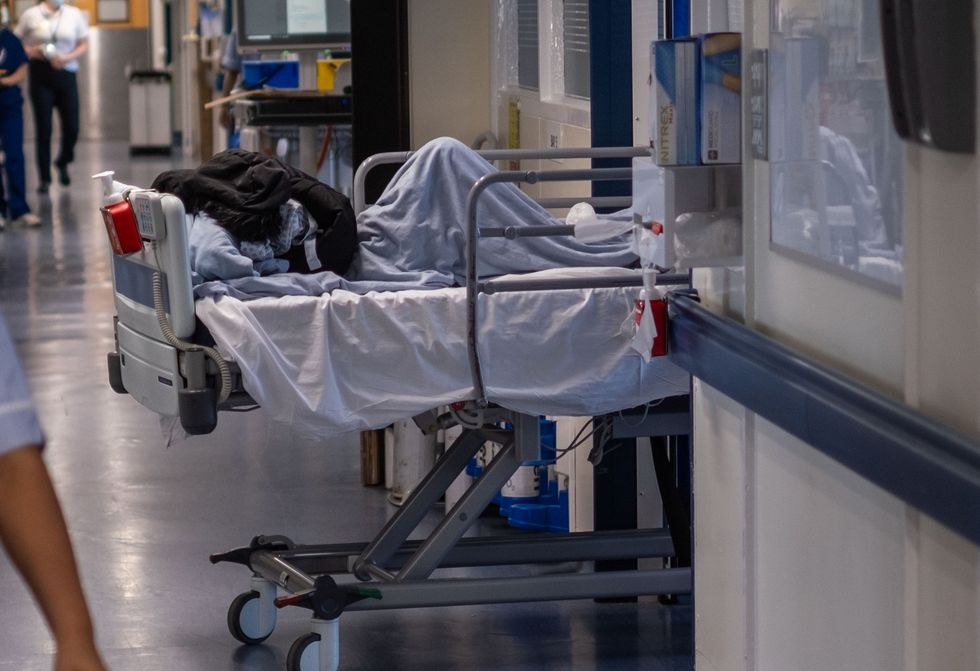
Corridor care is now an everyday practice in the NHS
|PA
Hospitals told investigators demand exceeds capacity year-round, driven by delayed discharges, ambulance handover pressures and a lack of social care and community support.
Temporary care environments include hospital corridors, waiting rooms, chairs on wards, upright and reclined seating areas, converted storage rooms and even ambulances parked outside emergency departments.
Many patients described distressing consequences.
Some spoke of difficulties with washing and toileting in public spaces or having invasive treatments carried out with little or no privacy.
One elderly patient said: “The corridor is busy, non-stop. I take a long time to get out of bed and am unsteady on my feet and need help moving around. When it is busy, it’s much harder [to move around] and I’m scared I’ll get knocked off my feet.”
Another said: “I don’t like to make a fuss because there are lots of sick people here and the nurses are run off their feet …”
LATEST DEVELOPMENTS:

Many patients have described distressing consequences of corridor care
|PA
Patients also said getting in and out of bed in busy corridors was particularly difficult for older and frail people.
While staff often tried to escort patients to toilets or side rooms for personal care, patients said that when staff were stretched there was sometimes no one available to help - leaving some patients having to hold on, or soil themselves.
The HSSIB warns corridor care creates patient safety risks that are harder to manage than in proper ward settings.These include:
- Difficulty monitoring patients and recognising deterioration
- Insufficient staff-to-patient ratios
- Increased infection risk
- Lack of piped oxygen and suction
- Compromised response to medical emergencies
- Fire and evacuation risks
In several cases, investigators were told of patients collapsing in corridors where there was no emergency buzzer to summon help quickly.
A senior nurse said: “I have had a patient collapse on me and been unable to pull an emergency buzzer as there are none. I had to shout and wait until someone heard me. Every second in that situation feels like a lifetime, managing the situation alone and the sense of relief when someone hears you is immense.”
The investigation raised serious concerns about delays in emergency response when patients are cared for in spaces not designed for acute treatment.
The report also warned that oxygen cylinders placed under trolleys may be used instead of piped oxygen, with the risk they could run out without staff noticing.
The report highlights research showing that some children and patients with mental health needs have also experienced care in temporary care environments in emergency departments.
At one hospital visited as part of a separate HSSIB investigation into mental health crisis, patients described being fearful because several people in mental health crisis were shouting and pacing around the department.
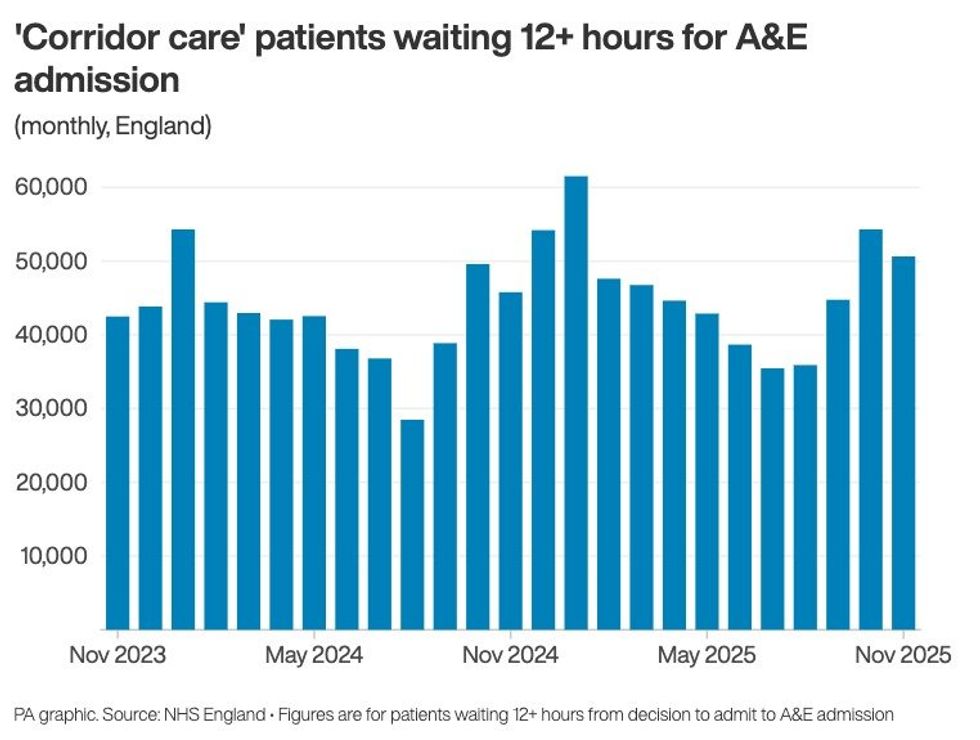
Number of 'corridor care' NHS patients waiting 12+ hours for A&E admission
|PA
These patients were awaiting Mental Health Act assessments or admission to inpatient mental health wards.
One patient who had attended A&E with new onset headaches left altogether because she felt “scared” and said “it was too noisy”.
Doctors and nurses told investigators corridor care is causing significant emotional harm.
Many said caring for patients in spaces not designed for treatment goes against everything they were trained for but despite the risks, staff described corridor care as the “best worst” option available.
Leaving patients unseen in waiting rooms, stranded in ambulances or waiting in the community was viewed as even more dangerous.
Hospitals described “spreading the risk” across wards and corridors to free up ambulances so they could respond to strokes, heart attacks and other emergencies.
But the watchdog warns this constant trade-off has now become routine rather than exceptional.
The investigation found stark differences in how hospitals are responding.
Some senior hospital leaders have now even adapted corridors and temporary areas to function more like standard wards, installing plug sockets, emergency call bells, communication systems and nearby equipment to reduce risks.

The report found corridor care is now year-round
|PA
It also confirms corridor care is now year-round, with little sign of relief unless patient flow improves.
The HSSIB is calling for a nationally agreed definition of temporary care environments and better data collection to understand their true impact.
Senior safety investigator Saskia Fursland said: “Until there is a solution to the complex underlying issues related to patient flow, we must recognise that hospitals may have no choice but to use temporary care environments.”
She added that by working together, NHS leaders could better understand and manage the risks involved.
The Royal College of Physicians said the report confirms what doctors are seeing daily.
Dr Hilary Williams, its clinical vice president, said: “Despite the best efforts of staff and providers, patients across the NHS are receiving treatment in corridors and spaces that were never intended for care delivery. These conditions are unacceptable, and this HSSIB investigation rightly highlights serious concerns relating to patient safety, as well as their dignity and experience.”
She said patients are being treated “without access to the basics like food, water and privacy”, while doctors experience “moral injury and very real emotional trauma”.
In a recent RCP survey, 94 per cent of physicians said patients’ privacy and dignity were compromised, and 53 per cent said patient safety was compromised.
Dr Williams warned: “Corridor care risks fundamentally undermining the public’s trust in the health service.”
The college is calling on the Government to publish promised data on corridor care “without delay”.
A Department of Health and Social Care spokesperson said: “No one should receive care in a corridor - the situation we inherited is unacceptable and undignified, and we are determined to end it.
“That is why NHS England is working closely with trusts to reduce variation, tackle inconsistencies, improve data collection and reduce discharge delays, alongside social care colleagues.
“Staff are under immense pressure, and this report highlights the dedication and professionalism of those who are keeping patients safe and delivering the best care they can.
“We know there is a long road ahead. This year we began preparing for winter earlier than ever before, delivering hundreds of thousands of extra vaccines to reduce pressure on hospitals, and investing £450million to expand urgent and emergency care, deploy 500 new ambulances and build 40 new mental health crisis centres so patients can get the care they need, when they need it.”
Professor Carl Heneghan, Director of Oxford University's Centre of Evidence Based Medicine said the language used in the report risked disguising a long-standing failure.
“The use of the term ‘Temporary Care Environments’ is a disgrace and an attempt to normalise corridor care,” he said.
He pointed out that when Tony Blair launched The NHS Plan in July 2000, the Government committed to ending the treatment of patients on trolleys in hospital corridors.
That pledge, part of a programme of NHS investment, staffing increases, and waiting-time targets included a commitment to ensure no patient would be treated on a trolley in a corridor by 2024.
Our Standards: The GB News Editorial Charter