'Potential disaster!' Half of NHS trusts using non-doctors as doctors

GB NEWS
In one high-profile case, Emily Chesterton died after a misdiagnosis by a physician associate, whom she mistakenly believed was a GP
Don't Miss
Most Read
Latest
Almost half of NHS hospital Trusts are now using non-doctors to fill doctors’ roles, new research shows, sparking a major safety warning from the British Medical Association.
The doctors’ union says patients are being put at risk as under-qualified staff are drafted in to plug rota gaps - describing the approach as “haphazard” and warning it could lead to a “potential disaster”.
In a new finding, freedom of information requests sent to hospital Trusts and Boards across the UK reveal that almost half are now allowing non-doctors onto doctors’ rotas.
Of those who responded, 41 said “yes” when asked if Advanced Practitioners were being used to plug gaps - compared to 44 who said “no”.
Advanced Practitioners - sometimes known as physician associates or specialist clinicians - come from a range of backgrounds, including nursing, paramedics and pharmacy.
They can play an important role in patient care when used appropriately.
But the BMA says NHS bosses are now going too far - pushing these staff beyond their training and into jobs that should only be carried out by fully qualified doctors.
Dr Tom Dolphin, chair of BMA council, said: “Our colleagues in advanced practice roles are valued members of our multidisciplinary teams.

Advanced Practitioners - sometimes known as physician associates or specialist clinicians - come from a range of backgrounds, including nursing, paramedics and pharmacy
| GETTY“Yet our research reveals an NHS management that will risk patient safety to push these professionals out of what they do best and use them as spare capacity to fill up understaffed doctors’ rotas.”
And he warned: “While other healthcare roles can be enhanced within safe limits, this must never encroach into areas where a doctor’s specific training and expertise is required.”
The figures expose what the BMA calls a postcode lottery in patient care - where treatment could depend on where you live.
“What is especially concerning is just how slapdash the NHS’s approach is,” Dr Dolphin said.
“Many employers have clearly and sensibly told us they would not put a non-doctor into the role of a doctor. Others have unashamedly responded that they have done exactly that.
“That these responses split almost down the middle is an indictment of an approach by Trusts and the NHS which means that where you live determines whether you will be seen by a doctor or by someone else for the same condition.”
The warning comes amid mounting pressure on the National Health Service, which is grappling with staff shortages, record waiting lists and rising demand.
LATEST DEVELOPMENTS:
Critics say the use of non-doctors in doctor roles risks blurring professional lines - leaving patients confused about who is treating them and what level of care they are receiving.
“This is a potential disaster for everyone involved,” Dr Dolphin added.
“Advanced practitioners are being asked to do jobs they shouldn’t have to. Patients are being given no clarity about who is treating them and what level of care they’re meant to be getting. Doctors are being left unclear on where the lines are drawn.
“The whole thing is a haphazard mess brought on by an absence of workforce planning and rational thinking about who can do what.”
In one high-profile case, Emily Chesterton died after a misdiagnosis by a physician associate, whom she mistakenly believed was a GP.

Critics say the use of non-doctors in doctor roles risks blurring professional lines
| PAThe 30-year-old, who lived in London, was repeatedly told her calf pain was a sprain, when she actually had a blood clot when she visited a GP practice in north London in October 2022.
She was not referred for further tests and died days later.
Coroners have also issued Prevention of Future Deaths reports highlighting cases where non-doctor clinicians did not properly assess deteriorating patients raising wider concerns about decision-making, supervision and the level of clinical expertise available on the front line.
“Patients deserve a consistent standard of care whichever hospital they happen to live near,” Dr Dolphin said.
“They shouldn’t have to worry about whether the local managers have asked non-doctors to deliver care that only uniquely-qualified doctors can safely deliver.”
At the heart of the row is a growing debate about the future shape of the NHS workforce.
With thousands of doctor vacancies unfilled, health bosses have increasingly turned to alternative roles to plug the gaps.
Physician associates and advanced practitioners have been rapidly expanded in recent years as part of long-term workforce plans.
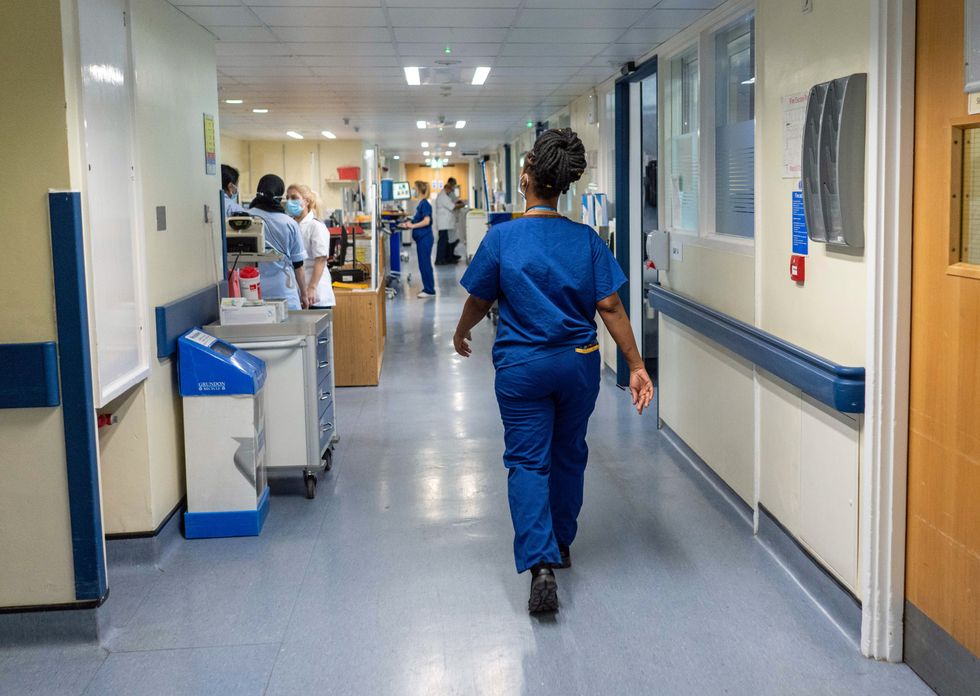
Physician associates and advanced practitioners have been rapidly expanded in recent years as part of long-term workforce plans
| PAHowever, critics argue the expansion has outpaced proper regulation - with unclear boundaries around what these roles can and cannot do.
The BMA is now calling for urgent action - including tighter regulation and nationally agreed limits on responsibilities.
“An NHS stretched to breaking point is no excuse,” Dr Dolphin said.
“Better regulation and clear, uniform scopes of practice to stop this blurring of professional lines are needed, so no patient comes to harm.”
An NHS England spokesman said: “NHS guidance is clear - advanced practitioners are highly skilled practitioners and are valued members of NHS teams alongside doctors.
“These roles should not replace the role of doctors and should only be used in line with their competence and qualifications, and all staff are able to raise concerns where they are worried about patient and staff safety.”
A spokesman for the Royal College of Nursing said: “Advanced nursing practice is highly-skilled, delivered by expert registered nurses and is underpinned by a master's level education and a comprehensive range of knowledge, skills and capabilities.
“These nurses are central to the delivery of safe and effective care across many services. They are not substitutes for other professions.
“They are autonomous professionals, delivering complex care as part of multi-disciplinary teams.”










