British scientists develop cheap malaria vaccine that could save millions
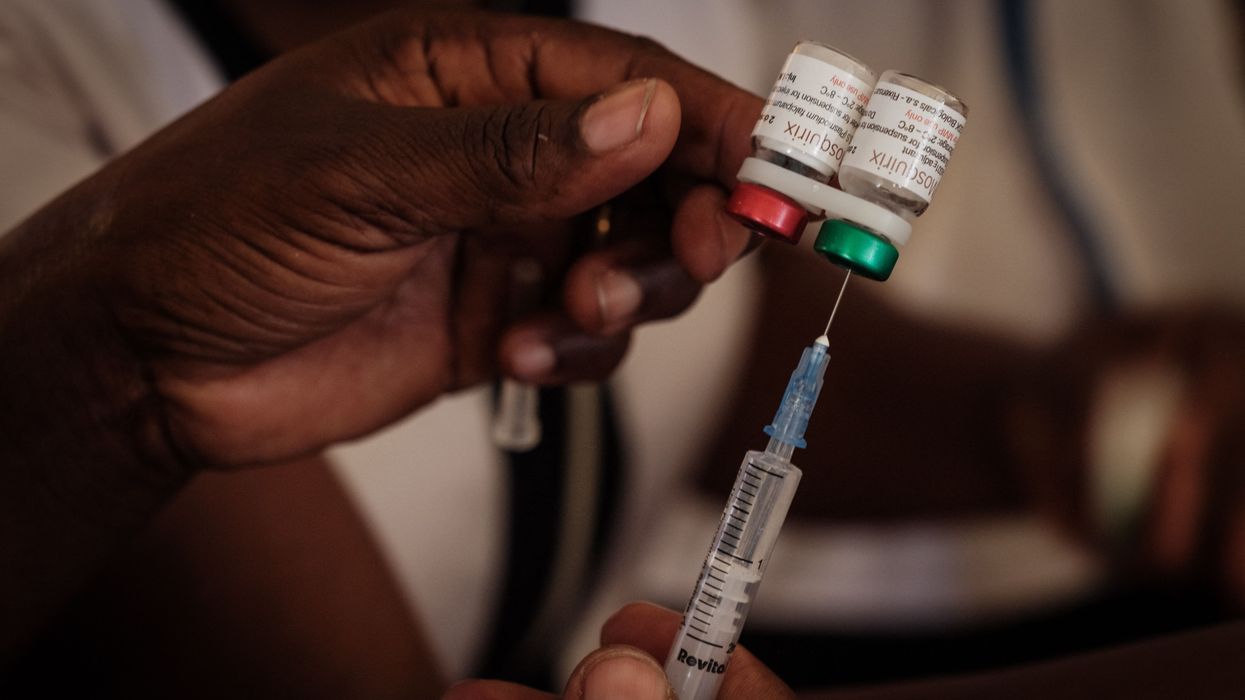
A nurse prepares a shot during the launch of the extension of the worlds first malaria vaccine
|GETTY

Agreements are in place to manufacture more than 100 million doses a year
Don't Miss
Most Read
A cheap malaria vaccine has been recommended for use by the World Health Organisation.
The announcement supporting the jab developed by the University of Oxford could save thousands of lives.
It is also only the second malaria vaccine to be developed.
Malaria is particularly fatal for babies and infants.

Malaria vaccine containers are stored in a cooler box
|GETTY
The scientific effort to tackle the scourge of malaria has been a long one.
The disease, which is spread by bites from mosquitoes, is hidden from the immune system by constantly shape-shifting inside the human body.
It is incredibly difficult to build up immunity naturally and difficult to develop an effective vaccine.
The WTO backed the first malaria jab, called RTS,S and developed by GSK, around two years ago.
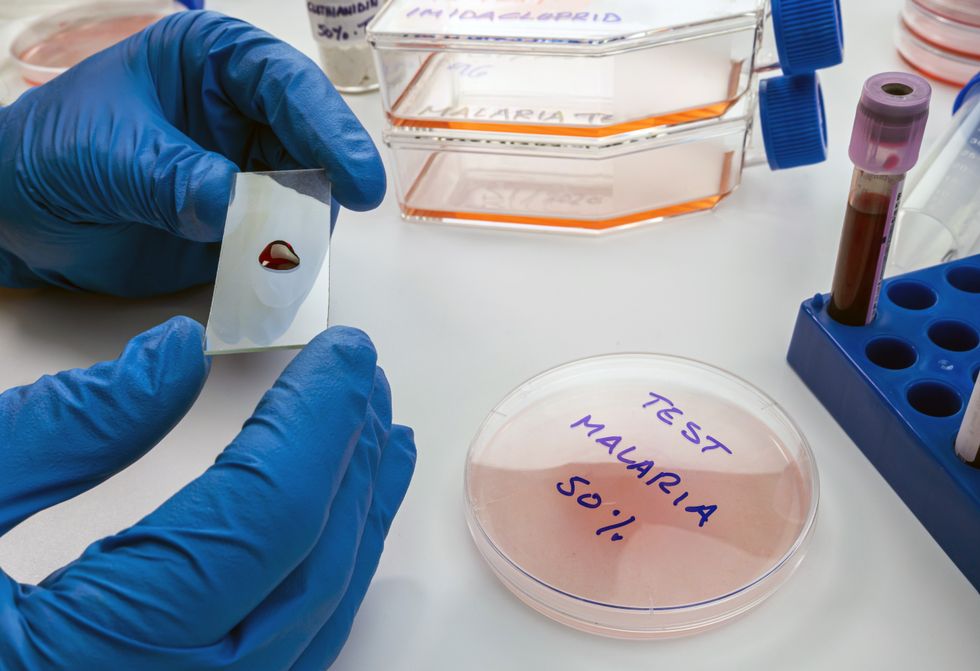
Conceptual image of a scientist examining blood sample from a sick person with malaria
|GETTY
WHO director-general Dr Tedros Adhanom Ghebreyesus celebrated the moment as a “great pleasure”.
He added: “I used to dream of the day we would have a safe and effective vaccine against malaria, now we have two.”
The two different vaccines have “very similar” efficiency rates but the R21 can be manufactured at a greater scale.
The WHO said the new R21 vaccine would be a "vital additional tool".
A stock image of a malaria vaccine
|GETTY
Each dose costs $2-4 (£1.65 to £3.30) and four doses are needed per person.
It is around half the price of the alternative RTS,S.
Malaria resulted in around 620,000 deaths in 2021, with a total of 247 million cases.
Cases are particularly prominent in Africa, where 95 per cent of malaria is found.

A mosquito from the side on a white surface
|GETTY
Dr Matshidiso Moeti, the WHO regional director for Africa, said: "This second vaccine holds real potential to close the huge demand-and-supply gap.
"Delivered to scale and rolled out widely, the two vaccines can help bolster malaria prevention, control efforts and save hundreds of thousands of young lives."
Professor Sir Adrian Hill, director of the Jenner Institute in Oxford where R21 was developed, said: "The vaccine is easily deployable, cost effective and affordable, ready for distribution in areas where it is needed most, with the potential to save hundreds of thousands of lives a year."
Gareth Jenkins, from Malaria No More UK, said: "The reality is that malaria financing globally is far from where it needs to be and annual deaths from malaria rose during the pandemic and are still above pre-pandemic levels, so we cannot afford to be complacent as new tools are developed."










